I have just returned from Old Fangak, Jonglei State, South Sudan after my fourth trip. I seem to have earned a welcome there for teaching bedside ultrasound to anyone who will learn and doing ultrasound whenever anybody asks. Also I cook a mean soup and make delicious chocolate sauce in which a homesick American can dip a piece of local deep fried bread dough.
The hospital I visit is a community health center which has morphed into a full service hospital for tens of thousands of people displaced by chronic civil war. Jill Seaman, a doctor friend from my home town and a champion of treatment for complex and fatal tropical diseases (particularly Kala Azar and tuberculosis), has coordinated the multiple functions of this center for years. It serves as a distribution point for food aid, a triage center for war wounded when the war is close by, a referral center for treatment of tuberculosis and Kala Azar and now a major outpost for Doctors Without Borders (Medecins sans Frontieres--MSF) in this area of the country. It also takes care of patients with rashes and fractures, splinters and pneumonia, delivers babies, nurses the dying and treats those with chronic diseases such as epilepsy, heart failure, asthma and sadness.
It sits on the bank of the Zaraf River, so named for the giraffes that roamed here before they were killed or driven off by war and hard times. The river is a beautiful slow moving thing that flows past the hospital on its way to the Blue Nile and then to Juba, South Sudan's horribly dysfunctional capitol city. Tropical birds of vast variety roost in the tamarind trees at the hospital and fish in the river, including egrets, kites and ibis. There is a vibrant open market, selling mostly cheap Chinese goods but also fish and locally grown vegetables, teas and nuts. (Also delicious dough creations for dipping in chocolate sauce when you get the chance.) The war seems always to be going on somewhere, but this year it was not too close. Still, nearly everyone has suffered some terrible loss.
My niche, other than cooking, is to teach ultrasound and be an internist. The ultrasound teaching is an extension of my enthusiasm for bedside ultrasound which is very useful in a place like this, where there are two portable ultrasound machines (one in French, through MSF) and no x-rays or CT scans. Being an internist has benefits too, since internal medicine is all about making sense of multiple complex symptoms or chronic diseases. I learn more tropical medicine each time I visit, but am hardly an expert. What I can do is recognize patterns of disease that can lead to effective treatments, and improvise treatment from what is available.
My trip in ultrasounds:
Before I arrived in Old Fangak, in the week before I left home, I got an email from Jill with a brief clip of an ultrasound of a boy's heart.
Jill sent the little ultrasound clip to the heart surgeons in Khartoum. They may be interested. It would be wonderful for her to have treatment at a dedicated pediatric heart surgery department in a major referral hospital because her heart is really weird and repairing may not be straightforward. Such a thing costs a lot of money, and she and her mother have none.
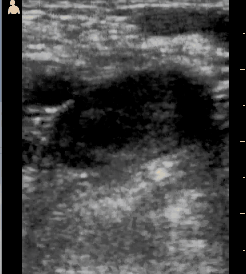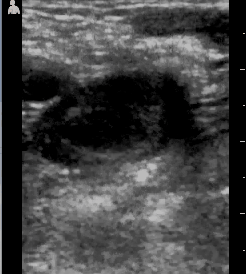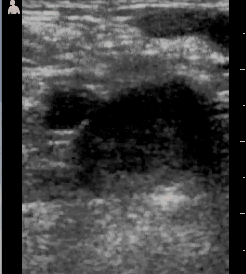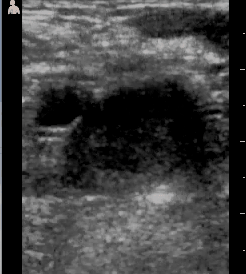
A patient who had fevers and had been in the hospital the previous week with them came to the clinic because he hadn't gotten better. He had an even higher fever and abdominal pain. His thin abdomen clearly had a lump in it. Ultrasound showed that it was a fluid filled mass about the size of a large grapefruit in his liver.
The lump was a liver abscess and in South Sudan the most common cause of this is an intestinal parasite called Entamoeba histolytica, or ameba for short. He was treated with a common antibiotic, metronidazole, and was significantly better the next day. His pain and his lump persisted, though. We worried that he might not be improving, but on the fourth day he felt much better and the lump, which had stayed big all this time, had shrunk to half its size. By the time I left he was looking like a normal guy. Small miracles.
An older lady was brought in by her grown daughters because of fever and pain. Tuberculosis most often presents as a lung infection in the US, but in Sub-Saharan Africa it is not at all uncommon for it to be primarily in other organs, even spread diffusely through the body and sparing the lungs. Her ultrasound showed clear lungs, but a collection of juicy lymph nodes near her aorta.
These would be likely to represent lymphoma in the US, but she probably has TB. Her daughter then pointed out that her leg was swollen. My second generation Vscan ultrasound has a transducer that can look at structures such as veins, and she had a big clot in the right leg, up to the groin. The central circular structure has some grayish material in it and doesn't collapse when I push, indicating that it is filled with clot.
A blood clot in the leg often suggests malignancy, and she may have cancer rather than TB, but TB can be associated with blood clots too! It was possible to order in a shipment of anticoagulant injections for her, and it was there within a few days, so she may be able to resolve the clot. She will not get lifelong blood thinners as she would in the US because it's just not practical. If she has TB, effective treatment may take care of her risk. If she has lymphoma her prognosis is not good.
There are rotating doctors through MSF who staff an emergency room, available to treat patients whose problems can't wait for clinic hours. Sometimes they would ask me to do an ultrasound when the diagnosis was a mystery. A teenage boy came in with the feeling that he couldn't urinate. He had had trouble with his bladder off and on for the previous year. When he had blood in his urine he was dosed with praziquantel, the anti-parasitic medication that treats schistosomiasis. Schistosomiasis is caused by a tiny organism that lives in bodies of fresh water, including the Zaraf River, and most of our patients have been infected by it. A single dose of praziquantel rids the body of the parasite, which can infect the bladder and cause inflammation and scarring. He had persistent irritation when he urinated so had then been treated for a standard bladder infection with antibiotics. He may have improved but his symptoms brought him back to the ER. He was miserable.
His ultrasound showed a round object that made a shadow right in the middle of his bladder. I've seen patients with bladder stones before, but they were always older men with large prostates or chronic urinary catheters. It turns out that bladder stones are not uncommon in the tropics in boys. I find nothing in the far reaching tubes of the internet that explains why, though a 1961 article suggests that there may be some nutritional factor involved. The surgeon rotating through MSF had seen the condition before and did a small operation to remove the stone. The boy was very pleased and showed me the gnarly egg sized thing on evening rounds.
There were other stories, medical and otherwise, and more ultrasounds. Pointing an ultrasound at patients with various illnesses taught me things I couldn't learn from reading. I think I infected some of the other doctors and clinicians with the urge to look inside with ultrasound, and the more they do the better they will get. Once again, it was a privilege to work with Jill and her dedicated staff and the other fellow travelers who swoop in and out like I do, trying to make a difference.
The hospital I visit is a community health center which has morphed into a full service hospital for tens of thousands of people displaced by chronic civil war. Jill Seaman, a doctor friend from my home town and a champion of treatment for complex and fatal tropical diseases (particularly Kala Azar and tuberculosis), has coordinated the multiple functions of this center for years. It serves as a distribution point for food aid, a triage center for war wounded when the war is close by, a referral center for treatment of tuberculosis and Kala Azar and now a major outpost for Doctors Without Borders (Medecins sans Frontieres--MSF) in this area of the country. It also takes care of patients with rashes and fractures, splinters and pneumonia, delivers babies, nurses the dying and treats those with chronic diseases such as epilepsy, heart failure, asthma and sadness.
It sits on the bank of the Zaraf River, so named for the giraffes that roamed here before they were killed or driven off by war and hard times. The river is a beautiful slow moving thing that flows past the hospital on its way to the Blue Nile and then to Juba, South Sudan's horribly dysfunctional capitol city. Tropical birds of vast variety roost in the tamarind trees at the hospital and fish in the river, including egrets, kites and ibis. There is a vibrant open market, selling mostly cheap Chinese goods but also fish and locally grown vegetables, teas and nuts. (Also delicious dough creations for dipping in chocolate sauce when you get the chance.) The war seems always to be going on somewhere, but this year it was not too close. Still, nearly everyone has suffered some terrible loss.
My niche, other than cooking, is to teach ultrasound and be an internist. The ultrasound teaching is an extension of my enthusiasm for bedside ultrasound which is very useful in a place like this, where there are two portable ultrasound machines (one in French, through MSF) and no x-rays or CT scans. Being an internist has benefits too, since internal medicine is all about making sense of multiple complex symptoms or chronic diseases. I learn more tropical medicine each time I visit, but am hardly an expert. What I can do is recognize patterns of disease that can lead to effective treatments, and improvise treatment from what is available.
My trip in ultrasounds:
Before I arrived in Old Fangak, in the week before I left home, I got an email from Jill with a brief clip of an ultrasound of a boy's heart.
This clip was taken by pointing an iPhone camera at an ultrasound machine and shooting a little video. It shows a normal boy's heart surrounded by a huge collection of fluid. The boy was short of breath, but had walked in. The condition had come on slowly. In Old Fangak, collections of fluid around the heart and lungs are usually due to tuberculosis and often respond quite quickly to a combination of steroids (prednisolone) and anti-tuberculosis medication. I told her that it was what she thought it was and that she should try her usual trick. Jill has gradually expanded her comfort with ultrasound beyond obstetrics but this was such a dramatic finding that she wanted another pair of eyes. When I arrived, this boy was one of the first patients I saw, and his pericardial effusion was almost gone about a week after starting treatment.
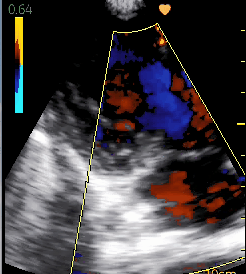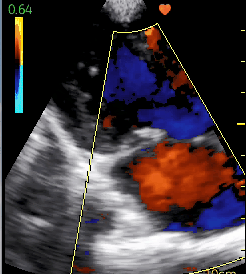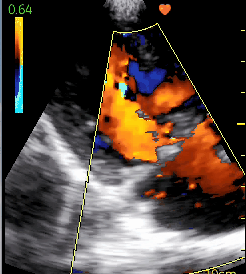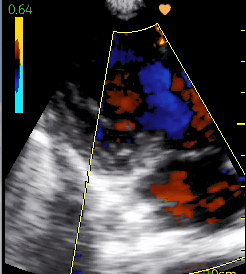
In the next bed in the hospital was another teenage boy with heart failure. He had been coming to the clinic for shortness of breath but despite medication had become so swollen and weak that he had been admitted. His ultrasound showed that his mitral valve was the problem.
Rheumatic fever is overwhelmingly a disease of poverty and lack of access to medical care. It starts with strep throat, then a few weeks later develops into an inflammation that can involve the heart. Years later the heart valves can become scarred. In his case, there is severe mitral stenosis, with very little blood flow through the valve separating the left atrium and ventricle, leading to stretching of the left atrium, abnormal heart rhythm and increased pressure in the vasculature of the lungs. Seeing this condition will lead to more appropriate medication and possibly even a heart procedure if he can get to the doctors in Khartoum (in the country of Sudan) who do free heart surgery.
Tuberculosis is common in South Sudan and the hospital at Old Fangak is a major treatment center for people who live with it. Patients who are diagnosed with TB take up residence in the TB compound in the village where they get daily observed treatment for the 6 months it takes to cure the disease. The compound is an area with a few buildings, a couple of latrines and enough flat ground for people to camp while they get their daily tablets. The patients get enough food, a mosquito net, a blanket and a dedicated though thinly stretched staff of mostly nationals who help them to survive while they get better. At clinic a few days after I arrived, a guy who was getting treatment for TB came in feeling short of breath even though he had been on appropriate treatment for a few weeks.
The ultrasound of his heart showed some thick stuff between the pericardium and the heart which doesn't allow the heart to fill properly. He had tuberculous pericarditis which had transitioned to a nasty constrictive effusive mess. He was treated with steroids in addition to his TB tablets which may reduce the inflammation and allow the heart to function properly. In a perfect world he would also have the option of surgery to remove the rind of constricting tissue.
A strikingly graceful and beautiful 6 year old girl came to clinic with her equally striking mother, troubled with breathing problems. She was able to walk long distances, but not fast and got out of breath easily. On exam she had a very loud heart murmur. It is not terribly uncommon to see congenital heart disease, and I expected that she had a ventricular septal defect (VSD), a hole in the wall between the two main chambers of the heart. When I looked with the ultrasound I saw nothing at all. Since her heart sounds were a little louder on the right side of her chest, I looked for her heart there. Sure enough, she was turned around. Her liver was on the left, heart on the right. And she did have a VSD.
A patient who had fevers and had been in the hospital the previous week with them came to the clinic because he hadn't gotten better. He had an even higher fever and abdominal pain. His thin abdomen clearly had a lump in it. Ultrasound showed that it was a fluid filled mass about the size of a large grapefruit in his liver.
The lump was a liver abscess and in South Sudan the most common cause of this is an intestinal parasite called Entamoeba histolytica, or ameba for short. He was treated with a common antibiotic, metronidazole, and was significantly better the next day. His pain and his lump persisted, though. We worried that he might not be improving, but on the fourth day he felt much better and the lump, which had stayed big all this time, had shrunk to half its size. By the time I left he was looking like a normal guy. Small miracles.
An older lady was brought in by her grown daughters because of fever and pain. Tuberculosis most often presents as a lung infection in the US, but in Sub-Saharan Africa it is not at all uncommon for it to be primarily in other organs, even spread diffusely through the body and sparing the lungs. Her ultrasound showed clear lungs, but a collection of juicy lymph nodes near her aorta.
There are rotating doctors through MSF who staff an emergency room, available to treat patients whose problems can't wait for clinic hours. Sometimes they would ask me to do an ultrasound when the diagnosis was a mystery. A teenage boy came in with the feeling that he couldn't urinate. He had had trouble with his bladder off and on for the previous year. When he had blood in his urine he was dosed with praziquantel, the anti-parasitic medication that treats schistosomiasis. Schistosomiasis is caused by a tiny organism that lives in bodies of fresh water, including the Zaraf River, and most of our patients have been infected by it. A single dose of praziquantel rids the body of the parasite, which can infect the bladder and cause inflammation and scarring. He had persistent irritation when he urinated so had then been treated for a standard bladder infection with antibiotics. He may have improved but his symptoms brought him back to the ER. He was miserable.
There were other stories, medical and otherwise, and more ultrasounds. Pointing an ultrasound at patients with various illnesses taught me things I couldn't learn from reading. I think I infected some of the other doctors and clinicians with the urge to look inside with ultrasound, and the more they do the better they will get. Once again, it was a privilege to work with Jill and her dedicated staff and the other fellow travelers who swoop in and out like I do, trying to make a difference.








Comments
It would have been interesting to analyze the mineral content of the bladder stone... & try making connections to dietary sources of the principal minerals.
When I read about the treatment of "chronic diseases such as epilepsy... and sadness" I admit to a little lump in the throat... and having to pause for a few moments before reading on. Bless you! ❤️
^..^